How do you stop the spread of infection?
Here’s a clear guide on stopping the spread of infection:
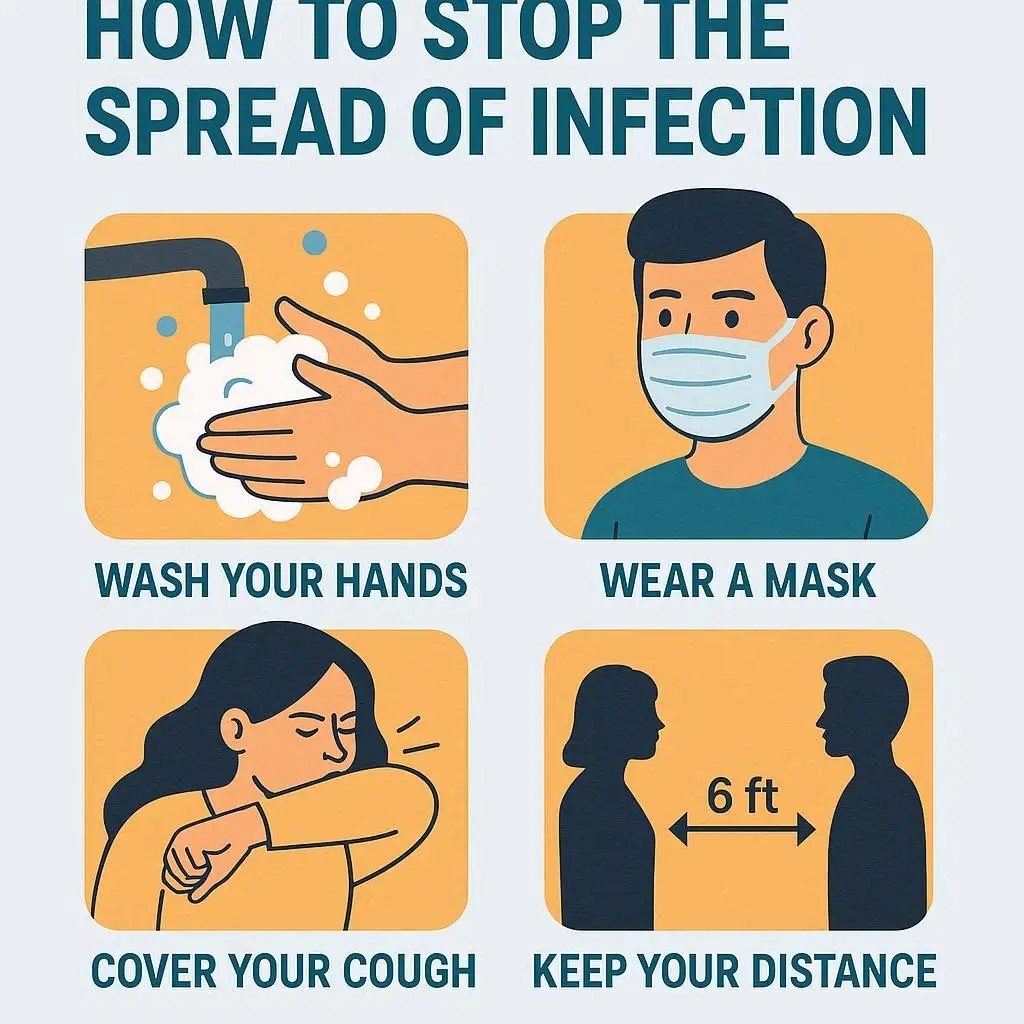
How to Stop the Spread of Infection: Key Prevention Tips
Infections can spread through direct contact, airborne droplets, contaminated surfaces, or bodily fluids. Preventing their spread is essential to protect yourself and others.
1. Practice Good Hand Hygiene
Wash hands frequently with soap and water for at least 20 seconds.
Use alcohol-based hand sanitizer when soap is not available.
Avoid touching your face, eyes, nose, and mouth with unwashed hands.
2. Cover Coughs and Sneezes
Use a tissue or elbow to cover your mouth and nose.
Dispose of tissues immediately and wash your hands afterward.
3. Wear Protective Gear When Necessary
Masks can prevent airborne transmission in crowded or high-risk areas.
Gloves may be necessary in healthcare settings or when handling contaminated materials.
4. Maintain Clean Environments
Regularly disinfect frequently touched surfaces such as doorknobs, phones, and countertops.
Ensure proper ventilation in indoor spaces to reduce airborne pathogens.
5. Practice Physical Distancing
Avoid close contact with people who are sick.
Stay home when feeling unwell to prevent infecting others.
6. Stay Up-to-Date with Vaccinations
Vaccines protect against preventable diseases (e.g., flu, COVID-19, measles).
Encourage family and community vaccination to reduce disease spread.
7. Promote Healthy Habits
Eat a balanced diet, stay hydrated, and get adequate sleep to strengthen immunity.
Regular exercise can also improve overall resistance to infections.
8. Educate and Raise Awareness
Share correct hygiene practices and infection prevention tips with family, friends, and the community.
Combat misinformation that can hinder prevention efforts.
Summary:
Stopping the spread of infection relies on a combination of personal hygiene, protective measures, environmental cleanliness, vaccination, and community awareness. Consistent practice of these habits can significantly reduce the risk of illness for you and those around you.
How Do You Stop the Spread of Infection?
Stopping the spread of infection is a collective effort built on simple yet powerful actions. Infections are primarily caused by germs (viruses, bacteria, fungi, parasites) that can spread from person to person through various routes, including direct contact, droplets from sneezes or coughs, or contaminated surfaces.
Key strategies include:
Hand Hygiene: This is universally recognized as the single most effective method.
Regular and thorough hand washing with soap and water, or using an alcohol-based hand sanitizer, removes or inactivates germs. Respiratory Etiquette: Covering your mouth and nose with a tissue or your elbow when coughing or sneezing prevents respiratory droplets from becoming airborne and infecting others.
Staying Home When Sick: Isolating yourself when experiencing symptoms of illness significantly reduces the chances of transmitting germs to others in workplaces, schools, and public spaces.
Cleaning and Disinfection: Regularly cleaning and disinfecting frequently touched surfaces (doorknobs, keyboards, phones, shared equipment) helps eliminate germs that can be picked up by contact.
Avoiding Touching Face: Germs often enter the body through the eyes, nose, and mouth, so keeping hands away from the face reduces self-inoculation.
What Are the Most Effective Infection Control Practices?
Effective infection control practices are multifaceted and are often categorized into "Standard Precautions" and "Transmission-Based Precautions."
Standard Precautions are the minimum infection prevention practices that apply to all patient care, regardless of suspected or confirmed infection status, in any healthcare setting.
Hand Hygiene: As mentioned, before and after all patient contact, after contact with body fluids, and after removing gloves.
Use of Personal Protective Equipment (PPE): Wearing gloves, gowns, masks, and eye protection as appropriate for the anticipated exposure.
Safe Injection Practices: Using a new needle and syringe for each injection and preventing needle-stick injuries.
Cleaning and Disinfection of Equipment: Reprocessing reusable equipment and regularly cleaning environmental surfaces.
Respiratory Hygiene/Cough Etiquette: Covering coughs and sneezes, and providing masks to symptomatic individuals.
Proper Waste Management: Safe disposal of sharps and other contaminated waste.
Appropriate Handling of Linen: Preventing contamination when handling soiled laundry.
Transmission-Based Precautions are used in addition to Standard Precautions for patients with suspected or confirmed infections that can be spread by airborne, droplet, or contact routes.
How to Implement Hygiene Protocols in Workplaces?
Implementing robust hygiene protocols in workplaces is crucial for creating a safe and healthy environment for employees and customers.
Develop a Clear Hygiene Policy: A written policy outlining expectations for both the company and employees regarding cleanliness, hand hygiene, and illness reporting is essential.
Promote Hand Hygiene:
Ensure easy access to handwashing stations with soap, water, and drying methods (paper towels or hand dryers).
Install numerous alcohol-based hand sanitizer stations throughout the premises, especially in high-traffic areas.
Use posters and regular communication to remind staff about proper handwashing techniques and when to wash hands.
Regular Cleaning and Disinfection Schedule:
Implement daily cleaning and disinfection of high-touch surfaces (doorknobs, light switches, shared equipment, desks, elevator buttons).
Schedule weekly or monthly deep cleaning for the entire facility.
Provide disinfectant wipes for employees to clean their personal workspaces, keyboards, and phones.
Encourage Sick Leave: Emphasize that employees should stay home when sick to prevent the spread of illness, without fear of penalty.
Improve Air Quality: Consider using air purifiers or improving ventilation to reduce airborne contaminants.
Effective Waste Management: Provide clearly marked bins for different types of waste and ensure regular emptying.
Employee Training and Awareness: Conduct regular training sessions on hygiene best practices and the rationale behind them.
Lead by example from management.
What Personal Protective Equipment Helps Prevent Infection?
Personal Protective Equipment (PPE) creates a physical barrier between individuals and infectious agents, reducing the risk of exposure and transmission.
Common types of PPE for infection prevention include:
Gloves: Protect hands from contact with blood, body fluids, mucous membranes, non-intact skin, and contaminated surfaces.
They should be single-use and disposed of after each interaction. Gowns/Aprons: Protect clothing and skin from splashes or sprays of infectious materials and prevent the soiling of personal attire during procedures or patient care activities.
Masks:
Surgical/Procedure Masks: Protect the mouth and nose from large respiratory droplets, splashes, or sprays.
They also serve as "source control" by preventing the wearer from spreading their own respiratory droplets. Respirators (e.g., N95, N99, N100):
Filter airborne particles and are used when there is a risk of inhaling very small infectious aerosols (e.g., tuberculosis, measles). Proper fit-testing is crucial for respirators to be effective. Powered Air-Purifying Respirators (PAPRs): Provide even higher levels of respiratory protection with a battery-powered blower.
Eye Protection (Goggles/Face Shields): Protect the eyes from splashes or sprays of blood or body fluids. Face shields offer broader protection for the entire face. Personal eyeglasses are not considered adequate eye protection.
It's crucial to remember that PPE is most effective when used correctly (donning and doffing procedures) and in conjunction with other infection control measures, not as a standalone solution.
How to Educate People About Infection Prevention?
Effective education is key to fostering a culture of infection prevention, whether in healthcare settings, workplaces, schools, or the general public.
Tailor the Message to the Audience:
Young Children: Use engaging methods like games, songs, visual demonstrations (e.g., glitter to show germ spread), and simple rhymes for handwashing.
Focus on basic actions like hand hygiene and not touching faces. Older Students/Adults: Introduce the link between personal behavior and public health, discuss modes of transmission, and provide data or case studies to show real-life impact.
Emphasize Key Behaviors: Focus on the most impactful actions, such as hand hygiene, respiratory etiquette, and staying home when sick.
Use Diverse Communication Channels:
Visual Aids: Posters, infographics, and clear signage in strategic locations (restrooms, entrances, common areas) can serve as effective reminders.
Digital Content: Videos, interactive online modules, and even educational games (like "Plague Inc.: The Cure" or CDC's "Solve the Outbreak") can make learning engaging.
Direct Training: Conduct workshops, webinars, or in-person training sessions, especially in professional settings like healthcare or food service, ensuring opportunities for questions and practical demonstrations.
Guest Speakers: Invite public health experts, doctors, or epidemiologists to share their insights.
Embed Lessons with Real-Life Connections: Discuss current health events, use the immediate environment to illustrate risks, and encourage critical thinking about how infections spread.
Lead by Example: Leaders and role models in any setting should consistently demonstrate good hygiene practices.
Provide Resources: Make reliable information (e.g., from CDC, WHO, local health departments) easily accessible.
Regular Reinforcement: Hygiene protocols should not be a one-time discussion. Regular reminders, updates, and refreshers help maintain awareness and compliance over time.
By understanding how infections spread and consistently applying these prevention strategies, we can all contribute to healthier communities.